EARLY DETECTION
Prostate cancer: what Swiss men need to know about symptoms, screening, and catching it early

Written by
Nick Lenten

Reviewed by

Every year, roughly 7,400 men in Switzerland are diagnosed with prostate cancer. It is the most common cancer in Swiss men. Caught early, it is highly treatable. The difficulty is that it grows silently. Most men feel nothing until the disease has already advanced.
This article covers the symptoms worth knowing, the screening tools that actually work, the risk factors that matter, and how advances in MRI and blood testing have reshaped early detection for prostate cancer in Switzerland.
What is prostate cancer?
The prostate is a walnut-sized gland sitting below the bladder, responsible for producing seminal fluid. Cancer begins when cells start dividing without the usual controls.
Some prostate cancers are aggressive. Many are slow-growing tumours that can sit confined to the gland for years, never threatening a man's life. This unpredictability is precisely why early detection matters.
How common is it in Switzerland?
About 7,400 Swiss men are diagnosed each year
60% of cases occur in men over 65
Risk is rare before 40 and climbs sharply after 50
Peak diagnosis: ages 50 to 70
Symptoms: what to watch for
Early-stage prostate cancer usually produces no symptoms at all. When symptoms do appear, they frequently mimic benign prostatic hyperplasia (BPH), a non-cancerous condition. That overlap is exactly what makes screening indispensable.
Early-stage symptoms
These can signal localised prostate cancer, but are equally common with BPH or prostatitis:
Weak or interrupted urine stream
Frequent urination, especially at night (nocturia)
Difficulty starting or stopping urination
Feeling the bladder hasn't fully emptied
Urinary retention or incontinence
When cancer has spread
In the minority of cases where cancer has already spread beyond the gland at the time of diagnosis, symptoms may include blood in urine or semen, pelvic or lower back pain, bone pain, or unexplained weight loss. These presentations are uncommon in Switzerland, where most prostate cancers are now caught at an earlier stage.
Any persistent urinary changes or pelvic pain in men over 50 warrant medical evaluation. These symptoms do not confirm cancer, but they should not be ignored.
BPH vs. prostate cancer
BPH is extremely common and mimics early prostate cancer almost exactly.
Age group | Percentage affected by BPH |
|---|---|
51–60 | ~50% |
60–69 | ~70% |
70+ | ~80% |
Frequent urination, weak stream, incomplete emptying – BPH causes all of these. Without screening, there is no reliable way to tell them apart based on symptoms alone.
Risk factors
Age
The single biggest risk factor. Most diagnoses land between 50 and 70. Sixty percent of all cases are found in men over 65.
Family history
A father or brother with prostate cancer raises your risk substantially. The risk climbs further if multiple relatives were affected or if any were diagnosed young. Notably, a maternal history of breast cancer is also associated with increased prostate cancer risk, likely reflecting shared genetic pathways including BRCA mutations.
BRCA1 and BRCA2 mutations
These gene mutations, best known for their role in breast and ovarian cancer, also increase prostate cancer risk. BRCA2 carriers face a particularly elevated risk of aggressive disease.
Ethnicity
Men of African descent develop prostate cancer more frequently, tend to get more aggressive forms, and face higher mortality rates. Earlier screening is especially important in this group.
Lifestyle and environment
Emerging research links diet, obesity, and certain chemical exposures to increased risk. The evidence is still accumulating. Maintaining a healthy weight and a balanced diet is sensible regardless.
Screening methods
Early detection is the single most important factor in prostate cancer survival. Here is what is available in Switzerland today.
Digital rectal exam (DRE)
A physician examines the prostate's size, shape, and consistency. It can detect palpable abnormalities but misses a lot – small or deep tumours escape detection, and results vary significantly between examiners. Best used alongside other tools.
PSA test (prostate-specific antigen)
This blood test measures a protein produced by the prostate. Elevated levels can indicate cancer, but also BPH, prostatitis, or other benign conditions.
On accuracy: using a standard threshold of PSA ≥4.0 ng/mL, the test has a sensitivity of around 70–80% (meaning it misses roughly 1 in 5 cancers) and a specificity of around 60–70% (meaning a significant number of elevated results are not cancer). In practice, only about 25–40% of men who go on to biopsy after an elevated PSA are actually found to have cancer. PSA is better understood as a triage signal than a diagnosis.
That said, it has clear population-level value. PSA-based screening reduces prostate cancer mortality by up to 20% (ERSPC trial, 16-year follow-up), with longer follow-up suggesting a more modest 13% reduction. Its limitations – false positives triggering unnecessary biopsies, false negatives missing real disease – are exactly why combining PSA with mpMRI significantly improves what you can actually act on.
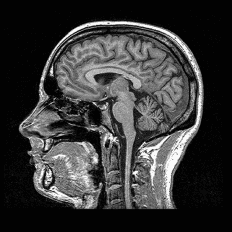
MRI: bi-parametric and multiparametric protocols
This is where prostate cancer detection has meaningfully advanced – and where it is worth understanding how MRI protocols differ, because the distinction matters practically.
Multiparametric MRI (mpMRI) combines three imaging sequences: T2-weighted imaging (anatomy), diffusion-weighted imaging (DWI, which reflects tissue density and cell behaviour), and dynamic contrast enhancement (DCE), which requires injecting a gadolinium contrast agent. mpMRI is the standard of care in diagnostic settings – when a man has an elevated PSA and needs a detailed workup before biopsy.
Bi-parametric MRI (bpMRI) uses the same T2 and DWI sequences but omits the contrast injection. No gadolinium. No IV line. Faster scan time. And for detecting clinically significant prostate cancer, bpMRI performs comparably to mpMRI. The PRIME trial, a 2025 multinational study of 490 men across 22 centres in 12 countries, confirmed noninferiority: bpMRI and mpMRI detected clinically significant prostate cancer at virtually identical rates (29.2% vs 29.6%), with sensitivity of 98.0% and 99.3% respectively. The authors concluded that bpMRI could become the new standard of care. The European Association of Urology endorses bpMRI as an appropriate first-line approach.
The logic is straightforward: contrast enhancement adds incremental value in diagnostically complex cases – equivocal lesions, prior treatment, recurrence – but provides limited additional benefit when the question is simply whether a clinically significant cancer is present in an asymptomatic man. For population-level screening, bpMRI may be the right protocol.
The PROMIS trial demonstrated what MRI-based detection achieves at population level:
MRI detected 93% of clinically significant prostate cancers; TRUS ultrasound caught just 48%
MRI avoided unnecessary biopsies in 27% of cases
MRI-based prostate screening is also considerably more comfortable than a digital rectal exam – which matters practically, because men who find screening aversive tend to delay or avoid it entirely.

Stockholm3 and other risk calculators
Several tools attempt to improve on PSA alone by combining it with additional biomarkers or genetic data. The Stockholm3 test, for example, incorporates free PSA, p2PSA, protein biomarkers, and genetic markers to generate a personalised risk score for aggressive disease. These tools can reduce unnecessary biopsies compared to PSA used in isolation. They are useful where PSA has flagged elevated risk and a more refined triage is needed – but they are a supplement to MRI assessment, not a substitute for it.
Prostate biopsy
Still the only way to definitively confirm prostate cancer. A physician extracts tissue samples for pathological analysis, guided by ultrasound or MRI. The PRECISION trial, a landmark 2018 study of 500 men across 23 centres, showed that MRI-targeted biopsy detected clinically significant prostate cancer in 38% of cases compared with 26% for standard TRUS-guided systematic biopsy. It also reduced detection of clinically insignificant cancers (9% vs 22%) and allowed 28% of men to avoid biopsy entirely when MRI
Stages
Stage | Description |
|---|---|
Stage I & II | Cancer confined within the prostate gland (localised) |
Stage III | Cancer has spread into nearby tissues beyond the prostate capsule |
Stage IV | Cancer has metastasised to lymph nodes, bones, or distant organs |
Most prostate cancers in Switzerland are caught at Stage I or II, where treatment outcomes are excellent.
Survival rates
Prostate cancer, when caught at a localised stage, has one of the highest survival rates of any cancer:
5-year survival rate: exceeds 90% across all stages
15-year survival rate for localised tumours: exceeds 97%, regardless of treatment type
The pattern is consistent across cancer research: find it early, and outcomes improve dramatically.
Treatment options
The right treatment depends on the individual: age, tumour grade and stage, genetic markers, overall health, and personal preference all factor in. In Switzerland, treatment decisions for prostate cancer are typically made through a multidisciplinary tumour board (Tumorboard) involving urologists, radiation oncologists, pathologists, and radiologists. This is standard practice, and any man facing a prostate cancer diagnosis should expect his case to be discussed by a specialist team.
Active surveillance
For slow-growing, low-risk cases: regular monitoring with PSA tests, DREs, and periodic MRI or biopsy. No immediate intervention.
Long-term data from the ProtecT trial supports active surveillance for low-risk disease, with important caveats. After 15 years, prostate cancer mortality was low across all three arms (surgery, radiotherapy, and monitoring). However, active surveillance is not the same as doing nothing: around half the men in the monitoring group eventually required surgery or radiotherapy during the follow-up period, typically when their disease showed signs of progression. The approach works because regular monitoring catches that progression early enough for curative treatment to remain effective.
After 10 years:
49% of men on active surveillance needed no treatment and showed no disease progression
Fewer than 2% developed metastases
Fewer than 1% died from prostate cancer
Radical prostatectomy (surgery)
Complete surgical removal of the prostate. A well-established treatment for localised cancer. The benefit varies considerably depending on age, tumour grade, and overall health. In some cases the survival advantage over monitoring is substantial; in others, particularly for older men with low-grade disease, the difference is marginal. Potential side effects include erectile dysfunction and urinary incontinence, both of which can often be managed.
Potential side effects include erectile dysfunction and urinary incontinence, both of which can often be managed.
Radiation therapy
Two main forms: external beam radiation (EBRT) and brachytherapy (radioactive seeds implanted in the prostate). Both are effective for localised and locally advanced disease, with survival outcomes comparable to surgery in many cases.
Hormone therapy (androgen deprivation therapy)
Prostate cancer feeds on androgens. Hormone therapy cuts androgen levels or blocks their effect. Used alongside radiation, for recurrent cancer, and for advanced or metastatic disease.
Chemotherapy
Reserved for metastatic prostate cancer no longer responding to hormone therapy. It slows progression and extends survival.
Focal therapy
Targets only the cancerous portion of the prostate, preserving healthy tissue. Techniques include cryotherapy, High-Intensity Focused Ultrasound (HIFU), and photodynamic therapy.
Immunotherapy
Sipuleucel-T (Provenge) is an FDA-approved cancer vaccine that stimulates the immune system to attack prostate cancer cells. Immune checkpoint inhibitors are effective for cancers with specific genetic markers (MSI-H or dMMR).
When to start screening in Switzerland
Screening is generally recommended from age 50 for men at average risk.
Earlier screening, from age 40 or 45, is appropriate for men with a family history of prostate cancer, African descent, or known BRCA1 or BRCA2 mutations.
Within the Swiss healthcare system, PSA testing requires a Hausarzt referral and is covered by Grundversicherung when clinically indicated. Advanced imaging such as mpMRI typically falls under Zusatzversicherung or self-pay.
In practice, proactive prostate screening is something many men have to advocate for themselves. GPs vary considerably in how readily they recommend screening before symptoms appear, particularly for men under 55 at average risk. If you want a prostate assessment before something prompts it, the clearest path is a preventive health assessment that includes it by design.
How Ahead Health supports early detection
Standard Swiss check-ups are reactive: they respond to symptoms or age thresholds. Prostate cancer doesn't wait for either. Ahead Health's preventive assessments are built for men who want a proactive baseline before anything prompts it.
The Ahead Advanced package (CHF 2,490) includes a full-body MRI using a bi-parametric protocol – T2-weighted and diffusion-weighted imaging, without contrast injection. For screening in asymptomatic men, this is the appropriate and evidence-supported approach: bpMRI performs comparably to full multiparametric MRI for detecting clinically significant prostate cancer, while avoiding the gadolinium contrast agent and keeping the scan faster. Crucially, it does far more than a prostate scan. The same session covers the entire body – organs, soft tissue, and blood vessels from head to pelvis – so you get a comprehensive picture of your cardiovascular health, abdominal organs, lymph nodes, and more, alongside the prostate assessment. It is a more comfortable alternative to a rectal exam, and a substantially broader one. The package also includes an 80+ biomarker blood panel covering PSA, metabolic markers, and gender-specific indicators.
The Ahead Core package (CHF 1,990) provides the full-body MRI and health report as a starting point if you want to begin with imaging alone, and you can add the prostate screening for CHF 150.
Every scan and blood result is reviewed by Swiss board-certified physicians and supported by AI-assisted analysis. The findings go to you and, if you choose, to your Hausarzt – complementing your GP's oversight rather than replacing it.
Supplementary health insurers may cover part of the cost. KPT, CSS, AXA, Visana and Atupri are all reimbursing part of the cost for Ahead Health services depending on their T&Cs, some with up to CHF 1,500. You can check how much you can get reimbursed and request a pro-forma invoice on our insurance page.
Conclusion
Prostate cancer is common, often silent, and highly treatable when found early. The 97% 15-year survival rate for localised disease is not a statistical abstraction – it is what early detection delivers. In Switzerland, where standard check-ups don't include advanced prostate imaging, a proactive assessment gives you the kind of baseline data that changes what's possible.
This article is for informational purposes only and does not constitute medical advice. Always consult a qualified healthcare professional for personal medical decisions.
FAQ
What are the first signs of prostate cancer?
At what age should I start prostate cancer screening in Switzerland?
What is a PSA test and how accurate is it?