EARLY DETECTION
Fatty liver disease: symptoms, causes, and how to detect it early

Written by
Nick Lenten

Reviewed by

One in three European adults has fatty liver disease. In Switzerland, the picture is similar. Most people have no idea.
The early stages produce few symptoms, sometimes none, and routine check-ups rarely catch it. A standard Grundversicherung appointment doesn't include liver imaging, and basic blood tests often miss early-stage fat accumulation entirely.
That silence is the problem. Undetected, a fatty liver can progress through inflammation, scarring, cirrhosis, and on to liver cancer or organ failure. Caught early, it is largely reversible through lifestyle changes alone.
Here is what fatty liver disease is, who gets it, how it is found, and what to do about it.
What is fatty liver disease?
Fatty liver disease – medically termed steatotic liver disease (SLD), or metabolic dysfunction-associated steatotic liver disease (MASLD) under the 2023 international consensus nomenclature – means excess fat has built up in liver cells. A healthy liver carries very little fat. When fat exceeds 5–10% of the liver's weight, the diagnosis applies.
The liver is the body's largest internal organ, driving metabolism, detoxification, protein synthesis, and bile production. Fat infiltration degrades all of these functions, often with no outward warning.
Two types: alcoholic and non-alcoholic fatty liver disease
Alcoholic fatty liver disease (AFLD)
Alcohol metabolism produces acetaldehyde, a toxic byproduct that damages liver cells and triggers inflammation.
Risk rises sharply with 30–50g of alcohol daily sustained over five or more years
Up to 90% of people consuming 60g+ daily develop early-stage AFLD
Europe has the highest global prevalence of alcohol-related liver disease
Progression runs from steatohepatitis to fibrosis to cirrhosis
Non-alcoholic fatty liver disease (NAFLD) / MASLD
NAFLD is the most common chronic liver condition in industrialised nations, developing in people who drink little or no alcohol. It tracks closely with obesity, insulin resistance, and type 2 diabetes.
Roughly 40% of men and 26% of women are affected
Up to 90% of people with obesity develop NAFLD; prevalence in those with type 2 diabetes reaches 55–70%
1 in 3 children with obesity already has the condition
Women with polycystic ovary syndrome (PCOS) face especially high exposure: 50–70% show signs of NAFLD
Can progress to non-alcoholic steatohepatitis (NASH) – now called metabolic dysfunction-associated steatohepatitis (MASH) – a more severe inflammatory form
How the disease progresses
Fatty liver disease follows a well-documented trajectory. Each stage is more difficult to reverse than the last.
Stage 1: Simple steatosis. Fat accumulates in liver cells without significant inflammation or damage. Fully reversible with lifestyle changes. Most people feel nothing.
Stage 2: Steatohepatitis (NASH or ASH). The liver becomes inflamed and cells sustain damage. Still reversible in many cases, but the margin for easy recovery is shrinking.
Stage 3: Fibrosis. Repeated inflammation replaces healthy tissue with scar tissue. Liver function declines measurably. Partial reversal may still be possible with aggressive intervention.
Stage 4: Cirrhosis. Severe, widespread scarring. Largely irreversible. Complications include portal hypertension, fluid accumulation, and cognitive impairment. In addition, hepatocellular carcinoma or liver cancer can develops in cirrhotic tissue – one of the fastest-growing cancer types globally.
Stage 5: Liver failure. The liver ceases to function when the cirrhosis progresses. Transplant becomes the only option.
Stages 1 and 2 are largely reversible. That is the entire argument for early screening.
Symptoms: what to watch for
Fatty liver disease earns the label "silent" for a reason. Screening catches what symptoms do not.
Early stage (often subtle or absent)
Persistent fatigue and general malaise
Mild pressure or discomfort in the upper right abdomen
Occasional loss of appetite
Difficulty concentrating
Advanced stage
As fibrosis or cirrhosis sets in, signs become harder to ignore:
Persistent abdominal pain and nausea
Jaundice (yellowing of skin and eyes)
Dark urine and pale stools
Abdominal swelling from fluid accumulation (ascites)
Confusion or altered consciousness (hepatic encephalopathy)
Easy bruising and prolonged bleeding
Rapid, unexplained weight loss and muscle wasting
Any of these advanced symptoms warrant immediate medical attention.
Causes and risk factors
Diet
A Western diet heavy in processed foods, refined carbohydrates, and sugary drinks is one of the strongest drivers. Fructose, particularly from sweetened beverages, is especially harmful – the liver is the primary organ responsible for metabolising it. Red meat promotes chronic inflammation and accelerates damage.
Body weight
BMI has a direct, dose-dependent relationship with fatty liver risk:
BMI up to 22: lower baseline risk
BMI 24.5+: risk approximately doubles
BMI 28.6+: risk increases sixfold
Fatty liver can also develop in people with normal BMI – "lean NAFLD" – due to genetic predisposition or visceral fat distribution. BMI alone is not a sufficient screening tool.
Physical inactivity
Sedentary behaviour is an independent risk factor. Sitting for 8 or more hours daily raises risk significantly, regardless of diet, weight, or exercise habits.
Alcohol
Sustained intake of 30–50g daily over years is the primary driver of AFLD. For reference, 20g of alcohol equals roughly one large beer, one glass of wine, or one shot of spirits.
Medications
Several drug classes can trigger or worsen fatty liver: corticosteroids, tamoxifen, irinotecan, and some antiretroviral medications.
Other factors
Chronic hepatitis C can independently cause liver fat accumulation. Genetic variants (notably in the PNPLA3 gene) significantly increase susceptibility. Hormonal imbalances – PCOS, hypothyroidism, and other endocrine disorders – elevate risk.
Diagnosis
Because early-stage fatty liver disease is asymptomatic, diagnosis depends on lab work and imaging rather than symptoms.
Blood tests and liver function markers
A comprehensive blood panel is the usual starting point:
Liver enzymes: GGT, AST, ALT – elevated levels signal liver cell damage
Lipid profile: triglycerides, total cholesterol, HDL, LDL
Fasting glucose and HbA1c: insulin resistance and diabetes risk
Complete blood count: overall health, exclusion of other conditions
Hepatitis B and C screening: rule out viral causes
Iron metabolism markers: check for hereditary hemochromatosis
The fatty liver index (FLI)
The Fatty Liver Index is a validated screening tool combining four measurements: BMI, waist circumference, GGT levels, and triglyceride levels. An FLI below 30 rules out fatty liver with high confidence; above 60 strongly suggests it. It works well as a first-line screen.
Imaging: ultrasound, elastography, and MRI
Ultrasound: widely available and non-invasive, but limited. It can miss early-stage disease and cannot reliably distinguish between stages.
Elastography (ultrasound- or MRI-based): measures liver stiffness, which correlates with fibrosis severity. A meaningful step up from standard ultrasound.
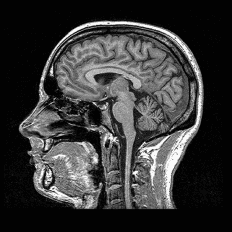
MRI: the most accurate non-invasive method for detecting and quantifying liver fat. It identifies fatty liver at the earliest stages and differentiates precisely between disease stages.
Liver biopsy
A needle extraction of liver tissue remains the definitive diagnostic reference. It is invasive, carries procedural risks, and is reserved for cases where non-invasive methods prove inconclusive.
Treatment and reversal
No FDA-approved medications exist specifically for fatty liver disease, though clinical research on GLP-1 receptor agonists is advancing. Lifestyle intervention remains the most effective, evidence-based approach.
Diet: the single biggest lever
High-protein intake: 60g of daily whey protein reduced liver fat by 20% in just four weeks in clinical studies
Low glycemic index foods: legumes, whole grains, nuts, seeds, and vegetables stabilise blood sugar
Omega-3 fatty acids: fatty fish (salmon, mackerel, sardines), walnuts, flaxseeds, olive oil, and avocados reduce liver inflammation
Fibre-rich foods: support gut health and reduce metabolic burden on the liver
Structured meal timing: three balanced meals per day with 5+ hour intervals; minimal snacking
Avoid or minimise: sugar-sweetened beverages, refined carbohydrates, processed foods, excessive red meat, and foods high in saturated fats.
Exercise
Physical activity reduces liver fat measurably, even without major weight loss:
150 minutes of moderate exercise per week significantly cuts liver fat
A combination of endurance and strength training works best
Changes in liver fat can appear within as little as four weeks
Weight loss
Losing 7–10% of body weight supports liver regeneration and significantly reduces fat content. Even 3–5% loss produces measurable benefits. Sustained, gradual reduction matters more than crash dieting.
Alcohol
For AFLD, complete abstinence is essential and often sufficient to halt or reverse early-stage disease. For NAFLD, limiting intake reduces the added metabolic load on a compromised liver.
Managing underlying conditions
Optimising blood sugar control in type 2 diabetes reduces liver fat. Managing cholesterol and triglyceride levels supports recovery. Treating insulin resistance through dietary and pharmacological interventions improves overall metabolic function.
Complications of untreated disease
Fatty liver is a systemic metabolic condition with consequences well beyond the liver:
Cardiovascular disease: heart attack, stroke, and coronary artery disease are leading causes of death in NAFLD patients
Type 2 diabetes: fatty liver both results from and accelerates insulin resistance
Chronic kidney disease: liver and kidney function are tightly linked
Obstructive sleep apnoea: strongly associated with NAFLD
Gallstone formation: altered bile composition raises gallbladder disease risk
Metabolic syndrome: a cluster of conditions that collectively multiply cardiovascular and metabolic risk
How Ahead Health detects fatty liver disease early
Swiss standard care does not include liver imaging as part of routine check-ups. The Grundversicherung covers basic liver enzyme tests, but these often miss early-stage fat accumulation, and they say nothing about the structural state of the organ. By the time abnormalities show up in routine blood work, the disease has often been progressing for years.
At Ahead Health, the assessment pairs two tools that work together: MRI imaging as the hardware layer, and comprehensive blood panels as the software layer.
The Ahead Advanced package (CHF 2,490) combines Ahead's full-body MRI – the gold-standard non-invasive method for quantifying liver fat – with an 80+ biomarker blood panel covering all key liver function markers: GGT, AST, ALT, lipid profiles, fasting glucose, HbA1c, and more. Combined with biometric measurements, these results yield your Fatty Liver Index and a complete metabolic risk profile. Every result is reviewed by Swiss board-certified physicians, with AI-assisted analysis to identify patterns that benefit from closer attention.
No single marker tells the whole story. Combining imaging with blood data gives you a picture that neither can provide alone.
Finding potential issues when they are small and manageable is the best time to find them. At Stage 1 or 2, reversal is still fully achievable. Later, it is not.
Supplementary health insurers may cover part of the cost. KPT, CSS, AXA, Visana and Atupri are all reimbursing part of the cost for Ahead Health services depending on their T&Cs, some with up to CHF 1,500. You can check how much you can get reimbursed and request a pro-forma invoice on our insurance page.
Conclusion
Fatty liver disease is common, largely silent, and reversible – but only if caught early. One in three European adults is affected. The structural damage progresses quietly for years before symptoms appear. By the time standard care flags it, the window for straightforward reversal has often passed. Proactive screening – liver MRI combined with a detailed metabolic blood panel – is the practical way to stay ahead of that trajectory.
FAQ
What is fatty liver disease?
What are the first signs of fatty liver disease?
Can fatty liver disease be reversed?